-
Understanding Reproductive Health: Common Conditions and Treatment Options
posted: Mar. 15, 2023.
Category: Women's Healthcare Reproductive health is important and if women are struggling with untreated reproductive health issues, it can affect their daily lives. It’s important that you’re able to identify if you might
Read more
Reproductive health is important and if women are struggling with untreated reproductive health issues, it can affect their daily lives. It’s important that you’re able to identify if you might
Read more
-
Signs of Abnormal Uterine Bleeding
posted: Mar. 01, 2023.
Female patients in Fountain Valley, CA, suffering from abnormal uterine bleeding should take this symptom seriously. Dr. Debora Sedaghat and her OC Women’s Care team are on-hand to assist with Read moreCategory: Obstetrics Gynecology Care, Women's Health Care, Gynecology -
What Can Cause Pelvic Pain?
posted: Feb. 28, 2023.
Category: Women's Healthcare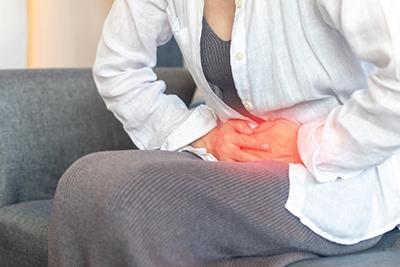 Dealing with pelvic pain can severely interrupt your normal routine. It can cause issues with your digestive, reproductive, or urinary system and can be incredibly disruptive. There are many issues
Read more
Dealing with pelvic pain can severely interrupt your normal routine. It can cause issues with your digestive, reproductive, or urinary system and can be incredibly disruptive. There are many issues
Read more
-
The Benefits of Regular Gynecological Exams
posted: Feb. 09, 2023.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Women's Health Care How often do you visit your gynecologist? If you don’t see your gynecologist at least once each year, you are missing out on an important way to protect your health.
Read more
How often do you visit your gynecologist? If you don’t see your gynecologist at least once each year, you are missing out on an important way to protect your health.
Read more
-
Navigating the Different Birth Control Options
posted: Jan. 26, 2023.
Category: Obstetrics Gynecology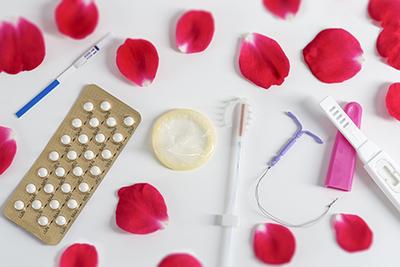 Having a baby is a wonderful experience, and it’s helpful to have a baby when you’ve planned on starting a family. Birth control can help prevent pregnancy, so you can
Read more
Having a baby is a wonderful experience, and it’s helpful to have a baby when you’ve planned on starting a family. Birth control can help prevent pregnancy, so you can
Read more
-
The Importance of Regular Gynecological Exams
posted: Jan. 13, 2023.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Women's Health Care, Gynecology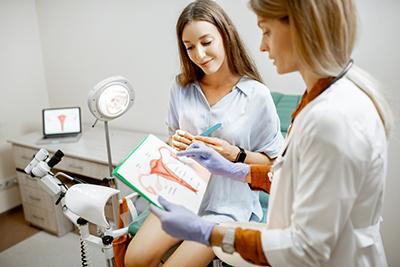 Your reproductive health is important. Regular gynecological exams can help protect your reproductive health and help prevent serious medical conditions like cervical cancer. Your OBGYN doctor is dedicated to protecting
Read more
Your reproductive health is important. Regular gynecological exams can help protect your reproductive health and help prevent serious medical conditions like cervical cancer. Your OBGYN doctor is dedicated to protecting
Read more
-
The Importance of Regular Gynecological Checkups for Women’s Health
posted: Dec. 29, 2022.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Women's Health Care, Obstetrics Gynecology Treatments, Gynecology If you are a woman, visiting your OBGYN doctor regularly for a checkup is one of the most important ways you can protect your reproductive health. Your OBGYN doctor is
Read more
If you are a woman, visiting your OBGYN doctor regularly for a checkup is one of the most important ways you can protect your reproductive health. Your OBGYN doctor is
Read more
-
Contraceptive Management
posted: Dec. 12, 2022.
Category: Obstetrics Gynecology, Gynecology It’s important to plan when you want to have a family. In order to keep from getting pregnant, you need to find a contraceptive that is right for you. Your
Read more
It’s important to plan when you want to have a family. In order to keep from getting pregnant, you need to find a contraceptive that is right for you. Your
Read more
-
Management of Abnormal Pap Smears
posted: Nov. 23, 2022.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Women's Health Care, Gynecology A pap smear is a routine test typically performed during a gynecological exam. It’s a test to determine the presence of abnormal or cancerous cells, specifically cervical cancer. Pap smear
Read more
A pap smear is a routine test typically performed during a gynecological exam. It’s a test to determine the presence of abnormal or cancerous cells, specifically cervical cancer. Pap smear
Read more
-
What Causes Pelvic Pain?
posted: Nov. 11, 2022.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Women's Health Care, Gynecology When you suffer from pelvic pain, it can be a scary experience. It’s only natural to wonder what is causing your pelvic pain. There can be a simple, benign cause,
Read more
When you suffer from pelvic pain, it can be a scary experience. It’s only natural to wonder what is causing your pelvic pain. There can be a simple, benign cause,
Read more
-
When to Visit an OBGYN
posted: Nov. 08, 2022.
Dr. Debora Sedaghat of OC Women's Care is here for you when you need an OBGYN in Fountain Valley, CA. An OBGYN or a doctor of obstetrics and gynecology can Read moreCategory: Obstetrics Gynecology, Obstetrics Gynecology Care -
FAQs About Hormone Imbalance
posted: Oct. 19, 2022.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Women's Health Care, Gynecology Your hormones handle a lot of important tasks to keep your body functioning. Unfortunately, there are a few life events which can cause your hormones to be out of balance,
Read more
Your hormones handle a lot of important tasks to keep your body functioning. Unfortunately, there are a few life events which can cause your hormones to be out of balance,
Read more
-
How an OBGYN Can Help With Infertility
posted: Oct. 05, 2022.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Obstetrics Gynecology Treatments If you and your partner have been trying to have a baby, but you are unsuccessful, have you thought about treatment for infertility? Your OBGYN doctor is an expert at
Read more
If you and your partner have been trying to have a baby, but you are unsuccessful, have you thought about treatment for infertility? Your OBGYN doctor is an expert at
Read more
-
The Importance of Annual Wellness Exams
posted: Sep. 23, 2022.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Women's Health Care A woman’s reproductive health requires special care, and that’s what an obstetrics and gynecology doctor does. These specialists, commonly known as OBGYN doctors, can help protect you from breast cancer,
Read more
A woman’s reproductive health requires special care, and that’s what an obstetrics and gynecology doctor does. These specialists, commonly known as OBGYN doctors, can help protect you from breast cancer,
Read more
-
What Are the Symptoms of Endometriosis?
posted: Sep. 12, 2022.
Category: Obstetrics Gynecology, Obstetrics Gynecology Care, Women's Health Care Do you double over in pain at the start of your period?
While cramps are a part of menstruation, what if we told you that going through bad cramps and pain
Read more
Do you double over in pain at the start of your period?
While cramps are a part of menstruation, what if we told you that going through bad cramps and pain
Read more
-
How an OBGYN Can Help
posted: Sep. 01, 2022.
Every woman deserves to feel comfortable and confident when she walks into medical appointments of such a sensitive nature. You want to have complete trust in the OBGYN providing your Read moreCategory: Obstetrics Gynecology
Blog
Contact Us
OC Women's Care
Office Hours
Monday:
9:00 am-5:00 pm
Tuesday:
9:00 am-5:00 pm
Wednesday:
9:00 am-5:00 pm
Thursday:
9:00 am-5:00 pm
Friday:
9:00 am-5:00 pm
Saturday:
Closed
Sunday:
Closed
